Nuna makes Value Based Care work. For everyone.
The operating system for Value Based Care: intelligent payment models, seamless operations, fast payments, engaged providers—powered by one platform
Value-Based MedEx per year on Nuna’s platform
17M
Lives impacted by the value platform & counting
26%
Higher shared savings for top providers accessing Nuna’s platform
6X
Faster payments and settlements
Value Based Care
needs a single platform

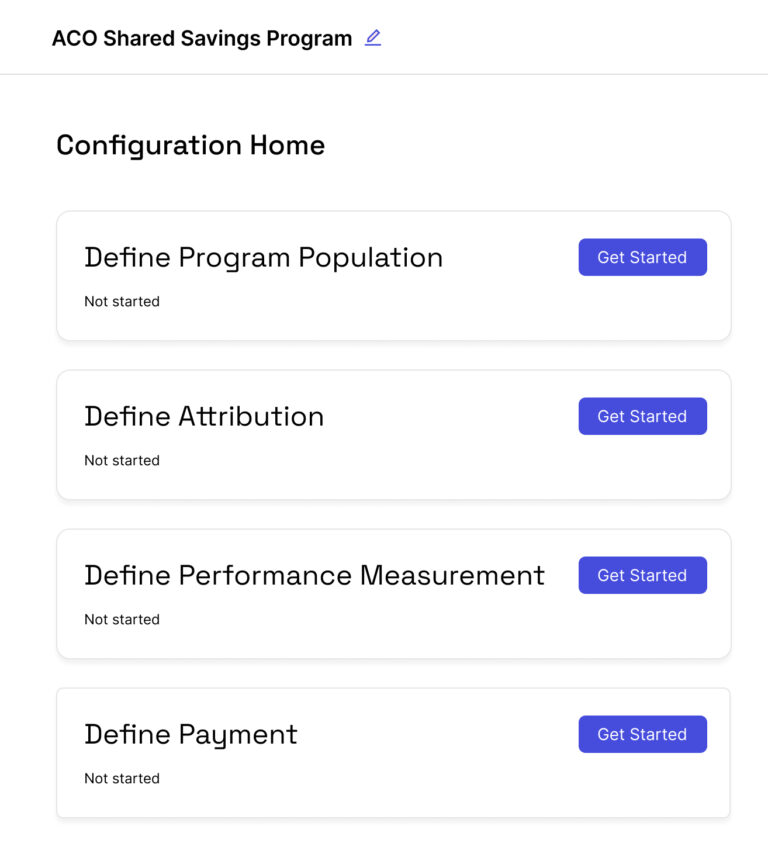
Administer and Innovate. Power all your Value Based Care Business, in one place.
Engage and inform providers so they can succeed across all your VBC Contracts.


Empower front-line Care Teams with specific action and incentive insights.
How we do it
We Get the Data Right
It starts with Nuna's Data Engine. Harmonizing and enriching all data to power your value-based payment models.
Design and Refine
Load your entire book of value-based programs and contracts. Refine and adjust, or design totally from scratch. Nuna's modeling and simulation does the heavy lifting, so you can do the innovating.
Operate and Pay, but Fast
Nuna's Platform removes the guesswork: Performance transparency, daily refreshes, dynamic reporting, and payments ledger, so you can pay and settle promptly.
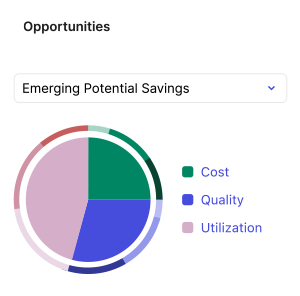
Activate with insights that work
Everyone wins and succeeds—deliver next-best actions, connected to value-based contract terms. Tap into Nuna's AI-driven predictions to ensure better outcomes.
Our Origins and Mission
“My earliest memories are of trying to navigate our healthcare system for my brother, Kimong. I founded Nuna for all the Kimong’s and families out there who deserve better.”

Join the Team
Nuna brings together preeminent talent across disciplines: engineers, data scientists, healthcare operations, security.
